Understanding Tooth Sensitivity After Filling for Months: Insights and Management
- 19 thg 11, 2025
- 4 phút đọc
Đã cập nhật: 16 thg 3
Tooth sensitivity is a common concern for many patients, particularly after dental procedures like fillings. When tooth sensitivity persists for months, it can be troubling for patients and may warrant examination from both a clinical and experiential perspective. This article delves into the causes, implications, and management strategies for tooth sensitivity after filling procedures, aiming to enhance understanding for both patients and dental professionals. Let's find out with Dental care knowledge through the following article.
What Is Tooth Sensitivity?
Tooth sensitivity, also known as dentin hypersensitivity, refers to discomfort or pain in the teeth when exposed to various stimuli, such as hot, cold, sweet, or acidic substances. It is characterized by a sharp pain that typically subsides once the stimulus is removed. For many patients, experiencing sensitivity following a dental filling is expected; however, prolonged sensitivity lasting months can indicate underlying issues.

Causes of Prolonged Sensitivity
This section explores the clinical underpinnings of tooth sensitivity following fillings, focusing on a few key factors:
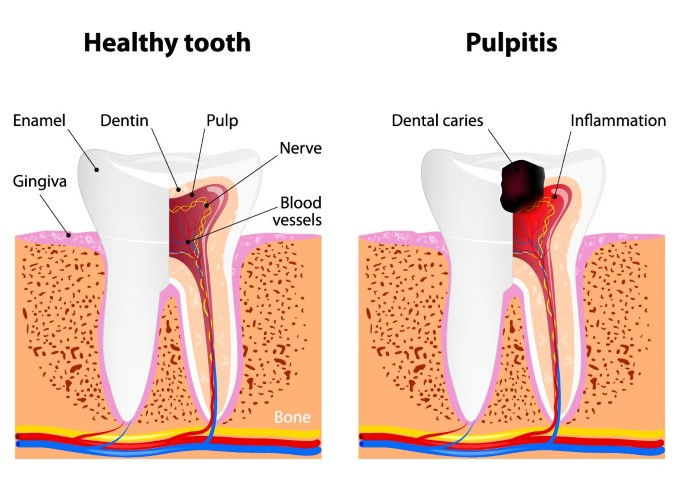
Nerve Irritation: Following a filling, the dental pulp, which houses the nerves of the tooth, may become inflamed or irritated. This can occur due to the nature of the filling material or the procedure itself. Studies have established that pulpitis (inflammation of the pulp) can lead to prolonged sensitivity, which can last from weeks to several months.
Microleakage: This term refers to the tiny gaps that can occur between the filling material and the tooth structure. These spaces can allow bacteria to enter, potentially leading to secondary caries or pulpitis. Research in dental health suggests that microleakage is a significant factor contributing to prolonged sensitivity after fillings.
Material Reaction: Different materials (e.g., composite resins, amalgam) can elicit varying responses in tooth sensitivity. For instance, composite resins may bond more effectively with moisture, allowing for better sealing; however, they can also expand or contract due to temperature changes, potentially leading to microleakage.
Lack of Post-Operative Care: Patient behavior post-filling can significantly impact sensitivity levels. For example, excessive consumption of acidic or sugary foods can exacerbate sensitivity. Combined with inadequate oral hygiene, the effects can lead to prolonged issues.
>>> See more: How to control sensitive teeth at home
Real-World Experiences
In numerous clinical settings, dentists have observed that patient experiences vary widely regarding tooth sensitivity after fillings. For instance, while some individuals recover swiftly, others report ongoing discomfort. A survey conducted across dental practices indicated that nearly 30% of patients experience sensitivity lasting over a month following the placement of a filling.
A notable case shared among dental professionals involved a 45-year-old patient who underwent a composite filling. Despite following proper post-operative guidelines, the patient reported sensitivity persisting for six months. Subsequent examinations revealed microleakage, which had gone undetected initially, leading to further treatment.
Clinical Data and Findings
Empirical studies shed light on tooth sensitivity post-treatment. Research published in the Journal of Dental Research illustrates that sensitivity can be influenced by various factors, including the type of filling used and the technique applied during the procedure.
One exploratory study analyzed the long-term effects of different materials on patient-reported sensitivity levels, revealing that resin-based composite fillings carried a slightly higher risk of prolonged sensitivity compared to amalgam fillings. Furthermore, a systematic review in the Cochrane Database of Systematic Reviews underscored the importance of proper filling placement techniques, highlighting that poorly executed procedures were correlated with higher rates of sensitivity.
Management Strategies
For dental practitioners and patients alike, managing prolonged tooth sensitivity is crucial for optimizing patient care and comfort. Here are evidence-based recommendations:
Desensitizing Agents: Over-the-counter products containing potassium nitrate or fluoride can significantly alleviate sensitivity. These agents work by obstructing the transmission of nerve signals or enhancing the enamel’s resistance to external stimuli.
Dietary Modifications: Patients should be guided to avoid highly acidic or sugary foods and drinks following fillings. Encouraging a diet rich in calcium and phosphate can help strengthen tooth structure.
Regular Follow-Ups: Dentists should schedule regular follow-up appointments for patients reporting prolonged sensitivity. This enables the timely identification of potential complications like microleakage or pulpitis.
Education and Communication: Patients should be educated on the normal timeline for recovery post-filling and informed about effective oral hygiene practices. Providing a comprehensive guide can enhance patient compliance and reduce anxiety.
Consideration of Filling Materials: When electing filling materials, dentists should assess each case individually, taking into account the patient’s specific conditions, such as existing sensitivities or prior dental experiences.
When to Seek Professional Help
Patients experiencing tooth sensitivity should seek professional evaluation if symptoms persist beyond three months. Persistent sensitivity might indicate severe issues such as:
Pulpitis: An examination may reveal underlying inflammation or infection that requires further intervention, such as endodontic therapy.
Cracked Tooth Syndrome: This condition can manifest as intermittent pain and typically necessitates advanced imaging and treatment.
Tooth sensitivity after fillings is a multifaceted issue that can arise due to several factors, with both clinical evidence and real-world experiences highlighting its complexity. By understanding the contributing aspects and incorporating effective management strategies, dental professionals can significantly improve patient outcomes. Continuous education and communication between practitioners and patients remain paramount in addressing this common yet often distressing post-operative experience.


Bình luận